At Region Vein, we recognize that vein treatment can feel overwhelming at first. That is why we guide you through each step with a clear, structured approach designed to make the process as comfortable and effective as possible.
Initial Consultation and Evaluation
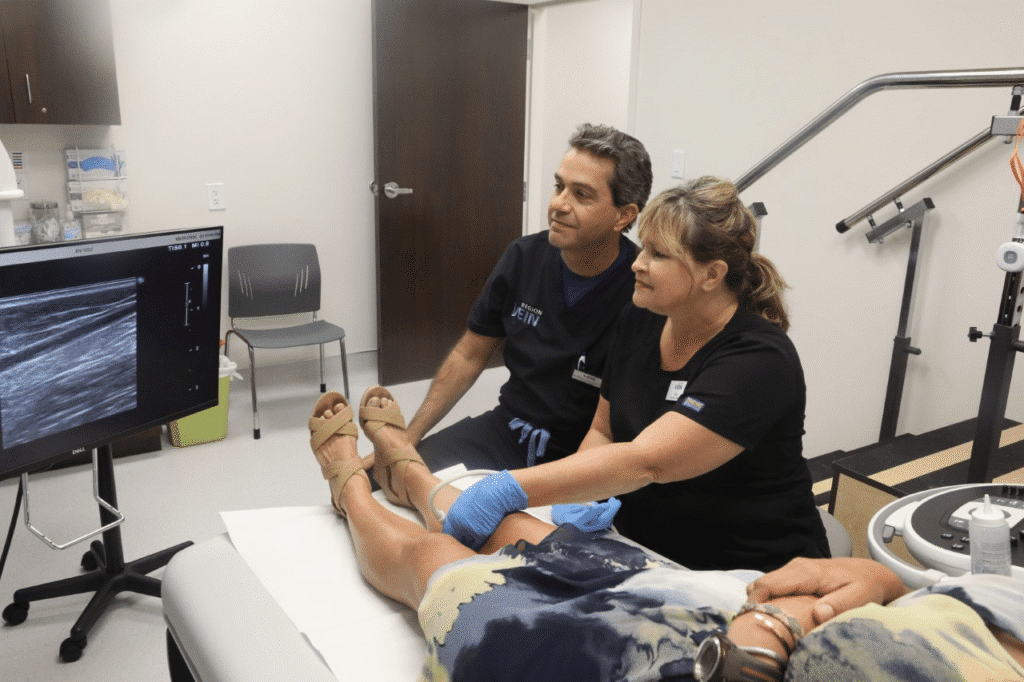
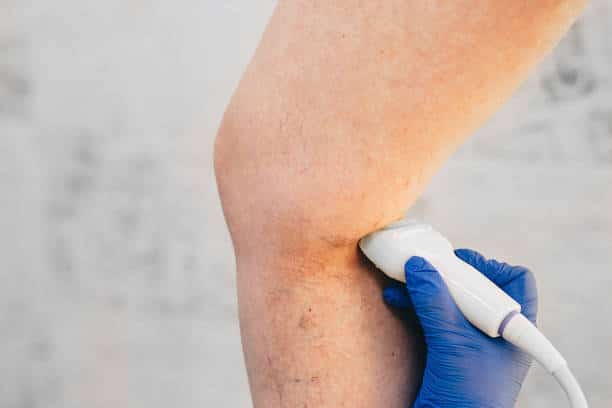
Your first visit to Region Vein centers around discussing your symptoms and finding their cause. During this appointment, we review your medical history, perform a physical exam, and assess any prior ultrasound findings. If needed, our experts may perform a more detailed ultrasound study to evaluate blood flow and pinpoint refluxing veins.
For patients with larger underlying vein issues, this advanced imaging helps confirm the most effective treatment strategy. If the concern is limited to smaller surface veins, additional mapping may not be necessary, and treatment options can often be discussed right away. At this stage, you will also receive a clear overview of potential treatments.
Common Questions During Your First Visit
Insurance coverage is one of the most common concerns. Our team will review your benefits, including deductibles and coverage for vein procedures. In many cases, treatment for larger varicose veins is covered, while cosmetic surface vein treatments may not be. If coverage is limited, we will provide a detailed cost estimate so you can plan accordingly.
Our billing specialists will walk you through the insurance approval process and answer any financial questions. Authorization timelines can vary depending on your insurance provider, ranging from a few days to several weeks. Some plans may also require documentation of conservative measures, such as compression therapy, before proceeding with treatment. Our team helps coordinate every step so you know what to expect.
Treatment Phase
Once evaluation is complete, treatment is carefully planned to address the root cause of your vein-related symptoms. Larger refluxing veins are typically treated first, as this is essential for long-term symptom relief and successful outcomes.
Depending on your condition, treatment may include conservative vein management, endovenous ablation, Varithena™, or sclerotherapy. After these primary veins are treated, any remaining branches or surface veins can be addressed with ultrasound-guided or traditional sclerotherapy. This step-by-step approach helps improve circulation while minimizing recurrence.
Why Choose Region Vein for Venous Treatment
Region Vein is built on a patient-first philosophy that emphasizes respect, compassion, and individualized care. Led by Dr. Demetrios J. Karamichos, a board-certified physician with over three decades of experience, the practice focuses exclusively on vein care using modern, minimally invasive techniques. His advanced credentials in venous and lymphatic medicine reflect a high level of expertise in both diagnosis and treatment.
Patients benefit from a highly personalized experience, supported by advanced technology and experienced ultrasound specialists who play an important role in accurate diagnosis and treatment planning. Every step of care is designed to be efficient, comfortable, and focused on long-term results, helping patients feel confident in both their care and outcomes.
Schedule Your Consultation
If you are experiencing symptoms of vein disease or have questions about treatment options, call our office at (219) 595-3095 to book your appointment with Dr. Demetrios J. Karamichos at Region Vein in Munster.